Guidance and Resources for Those with Axial Spondyloarthritis
Axial spondyloarthritis (AxSpA) encompasses a group of inflammatory arthritis conditions primarily impacting the spine, though other joints and even organs can be involved. We invite you to discover more about this range of conditions, their diagnosis and treatment options, and ways you can manage them effectively.
Living with axial spondyloarthritis (AxSpA) presents daily hurdles. There are two main types: radiographic axSpA, also known as ankylosing spondylitis, visible on X-rays due to damage to the sacroiliac joints and spine, and nonradiographic axSpA (nr-axSpA) which might not show on X-rays but can be detected through MRIs. We're here to guide you with expert advice, resources, and support to navigate through your AxSpA journey and alleviate its symptoms.
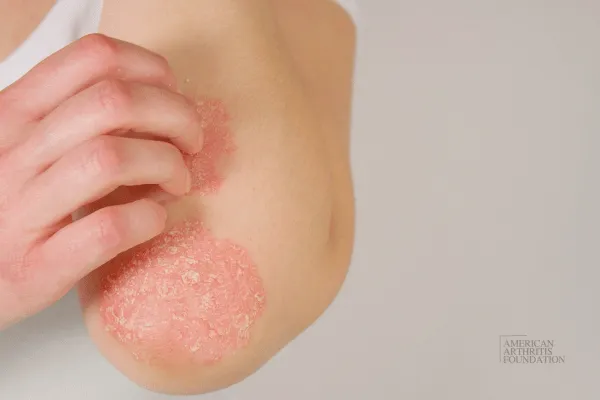
Understanding the Different Faces of Psoriatic Arthritis: New Study Reveals 3 Patient Clusters
Psoriatic arthritis (PsA) is a complex and often unpredictable condition that affects both the skin and joints. While some patients experience primarily joint-related symptoms, others face severe skin involvement due to psoriasis. But not all PsA cases follow the same path—and new research is helping us understand why.
A groundbreaking study published in the Annals of the Rheumatic Diseases has identified three distinct phenotype clusters among PsA patients, revealing key differences in disease presentation and response to treatment.
🔢 The Three Clusters of PsA
The researchers categorized patients into three unique groups based on the severity of their joint and skin symptoms:
Cluster 1: Mild PsA with Mild Psoriasis
✔️ Low joint involvement and minimal skin symptoms
✔️ Typically less severe disease progressionCluster 2: Severe PsA with Mild Psoriasis
✔️ High joint counts and more joint damage
✔️ Moderate but not severe skin involvementCluster 3: Severe PsA with Severe Psoriasis
✔️ Extensive psoriasis with high levels of systemic inflammation
✔️ Greater disease burden overall
📉 Why These Findings Matter
One of the most significant takeaways from this study is that patients in Cluster 3 (severe PsA with severe psoriasis) experienced the greatest improvements when starting or switching treatments. This reinforces the importance of taking both joint and skin symptoms into account when developing a treatment plan.
Traditionally, PsA treatment has focused on managing joint pain and stiffness. But this research highlights that skin severity should be considered equally important, especially when inflammation is widespread. A more comprehensive, personalized treatment strategy can help improve outcomes and quality of life.
💪 Toward Personalized PsA Care
This study aligns with the growing movement toward precision medicine in autoimmune care. By understanding the different ways PsA presents in patients, healthcare providers can:
📌 Tailor therapies to individual needs
📌 Monitor skin and joint symptoms in parallel
📌 Adjust treatments more effectively when patients aren’t responding
💡 What You Can Do
If you’re living with PsA, pay close attention to how your skin and joint symptoms interact. Share these observations with your healthcare provider and ask if your treatment plan reflects both aspects of your condition.
💬 Have you noticed a connection between your PsA flares and skin symptoms? Let us know in the comments or share your story to help raise awareness!

Have a question?
We're Here to Help
By providing my phone number, I agree to receive text messages from the business.


